New risk factors for rare childhood cancer
Researchers identify genes that can cause brain tumours in children and other cancers later in life
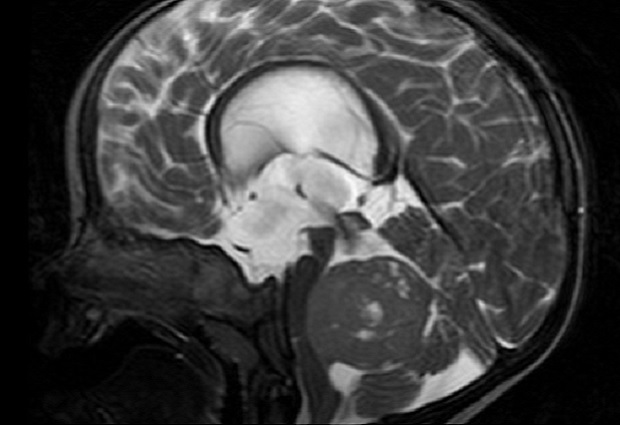
A research team led by EMBL scientists has found that five percent of children with a rare brain tumour called medulloblastoma develop the disease due to genetic risk factors. The genes involved can also be used to identify patients at high risk for additional cancers later in life. The Lancet Oncology publishes the findings on May 9.
Medulloblastoma is a rare malignant brain tumour typically diagnosed in children. Genetic factors were long suspected to play a role in its development, but information on which genes pose a risk for medulloblastoma was sparse. This meant there was no standard way to identify patients at risk of developing the disease.
EMBL scientists Jan Korbel and Sebastian Waszak, together with an international team of researchers from Germany, USA, and Canada (see below), have now been able to identify a set of genetic risk factors, based on analysis of 1022 patients with medulloblastoma.
Six genes
“We found that six genes are responsible for five percent of medulloblastoma cases, and up to twenty percent for one of the four known subgroups of medulloblastoma,” says Sebastian Waszak from EMBL Heidelberg, one of the study’s lead authors. “Among these genes are also risk factors that were already known to increase the risk of cancer in adults.” Defects in these genes can also lead to error-prone DNA repair during brain development. This results in brain tumours with a highly unstable genetic makeup, a phenomenon that is typically seen in cancers that occur later in life.
Interdisciplinary science
“This paper also reflects how science is becoming more interdisciplinary, with our research sometimes allowing medical doctors to take new paths,” adds EMBL group leader Jan Korbel. “The genetic risk factors we identified act as a biomarker, allowing for the identification of patients that are at high risk to develop breast and colon cancer after their successful cure from the brain tumour.”
The authors propose criteria for routine genetic screening in medulloblastoma patients, based on molecular tumour characteristics such as genetic instability. These findings are already changing the ways in which medulloblastoma patients are supported during and after their therapy.
The EMBL team collaborated with researchers from the German Cancer Consortium (DKTK), St. Jude Children’s Research Hospital in Memphis, the Hospital for Sick Children in Toronto, and Hopp Children’s Cancer Center at the NCT Heidelberg (KiTZ): a joint institution of Heidelberg University Hospital (UKHD) and the German Cancer Research Center (DKFZ).
The project was supported by the German Cancer Consortium (DKTK), German Cancer Aid, the German Childhood Cancer Foundation, and the Federal Ministry of Education and Research (BMBF).


