How new HIV drugs lock virus in immaturity
Study provides insights into workings of new HIV drugs and how virus becomes resistant
A new type of HIV drug currently being tested works in an unusual way, scientists in the Molecular Medicine Partnership Unit, a collaboration between EMBL and Heidelberg University Hospital, have found. They also discovered that when the virus became resistant to early versions of these drugs, it did not do so by blocking or preventing their effects, but rather by circumventing them. The study, published online today in Science, presents the most detailed view yet of part of the immature form of HIV.
HIV, the virus that causes AIDS, comes in two forms: immature and mature. The immature form is assembled inside an infected person’s cells. After an immature virus particle has left the cell, it has to change into the mature form before it can infect other human cells. A new group of drugs that inhibit this maturation is currently undergoing clinical trials, but so far it was unclear how exactly these drugs act.
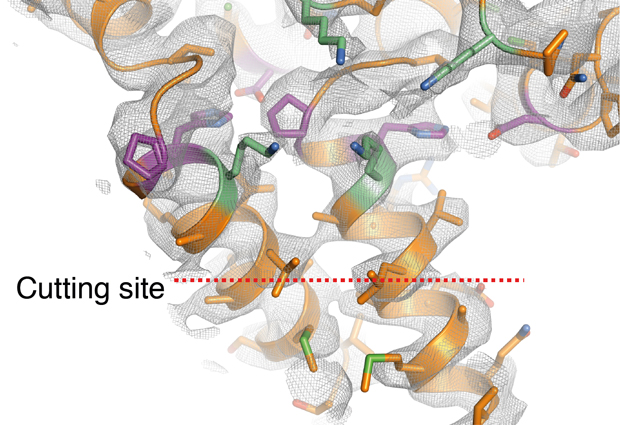
To go from immature to mature, HIV has to cut the connections between its main building blocks, and rearrange those pieces. John Briggs’ lab at EMBL and Hans-Georg Kräusslich’s lab at Heidelberg University Hospital looked at a particularly important cutting point. It connects building blocks known as the capsid protein and the spacer peptide 1, and if it is not cut, the virus cannot mature. The scientists used a combination of cryo-electron tomography and subtomogram averaging to reveal exactly what this part of the immature form of HIV looks like in 3D. They found that the cutting site is hidden in a position where the virus’ cutting machinery can’t sever it. So for the virus to mature, the structure first has to change, to expose that cutting point.
“When we looked at the virus with one of these inhibitor drugs on it, we found that the inhibitor doesn’t prevent the cutting machinery from getting in, as you might expect,” says Florian Schur, who carried out the work in Briggs’ lab. “Rather, the drug locks the immature virus structure in place, so that it can’t be cut.”

When the new inhibitor drugs were first developed, scientists found that HIV viruses with certain mutations in their genetic sequence were unaffected by the drugs – they were resistant. Having determined what the cutting point looks like and how the drugs act, Briggs and colleagues are now able to understand the effects of those mutations.
“Rather than stopping the drug from binding, the virus becomes resistant through mutations that destabilise the immature structure,” says Kräusslich. “This allows it to rearrange and be cut even when the drug is in place.”
The researchers would now like to probe the virus and the inhibitor drugs in even greater detail, to understand exactly how the drugs attach themselves to the viral proteins, and potentially gather data that could help to search for better drugs – or to design them.
The method used in this study – combined cryo-electron tomography and subtomogram averaging – enables scientists to study structures inside irregular viruses like HIV, or within cells. In essence, the scientists use an electron microscope to obtain a 3D image of the sample – in this case, whole HIV-1 particles. They then identify all the copies of the object they want to study – all the instances of the capsid protein-spacer peptide 1 cutting point – and use software to rotate the 3D image of each copy so that they are all facing the same way. By repeating this procedure with thousands of images, the scientists can obtain an accurate picture. With this approach, researchers can study such samples without having to purify them in a test-tube, which means that they see them in their real state. The EMBL scientists’ work now proves that the method can provide the level of detail that is crucial to understanding how molecular machines work and to informing drug design.



