€2.45 m to investigate leukaemia causes and therapies
The Heidelberg-based LeukoSyStem consortium investigates leukaemia stem cells in acute myeloid leukaemia. The German Federal Ministry of Education and Research financially supports this collaboration between Heidelberg University Hospital, HI-STEM gGmbH, the German Cancer Research Center and EMBL.
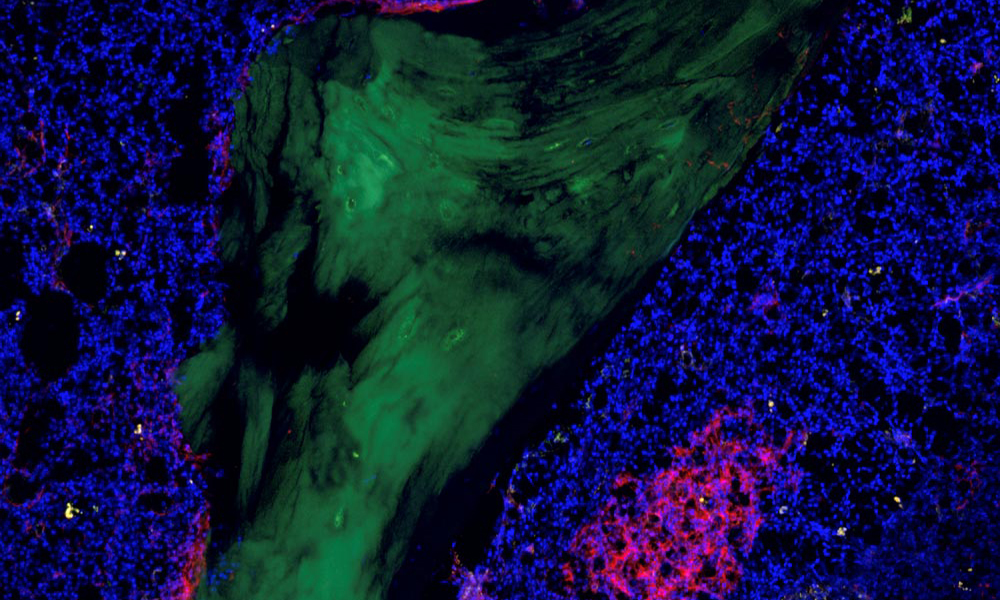
Leukaemia stem cells are considered to be the starting point of leukaemia; their elimination is a basic prerequisite for a successful long-term therapy. Scientists at Heidelberg University Hospital (UKHD), the Heidelberg Institute for Stem Cell Technology and Experimental Medicine at the German Cancer Research Center (HI-STEM/DKFZ), the German Cancer Research Center (DKFZ) and the European Molecular Biology Laboratory (EMBL) have now obtained research funding of €2.45 million from the German Federal Ministry of Education and Research (BMBF) as part of the junior research alliance LeukoSyStem. The aim of their project is to investigate the cells that are the origin of acute myeloid leukaemia (AML) and thus “get to the root of the problem”. The scientists intend to use isolated single cells from patient samples to investigate characteristic markers, mutations, functional data, and metabolic pathways, to gain a better understanding of leukaemia stem cells and their environment in bone marrow. The collected data will be evaluated comprehensively with the help of computer algorithms specially developed for the purpose.
Leukemia stem cells as the origin of a disease that is often fatal
The development of normal, healthy blood cells starts from haematopoietic stem cells in the bone marrow and proceeds through various stages of so-called precursor cells. In each of these stages, the accumulation of mutations can lead to cell degeneration and the development of blood cancer (leukaemia).
Acute myeloid leukaemia (AML) is the most common form of leukaemia in adults. In AML, mutated, functionless blood cells – known as blasts – overgrow other bone marrow cells. Every year in Europe, three to five out of every 100 000 people receive a diagnosis of AML. Despite therapeutic options such as chemotherapy and stem cell transplantation, relapses are frequent and the five-year survival rate for patients up to the age of 60 is 35–40%. For patients above 60, it is only 5–10%.
A basic prerequisite for the effective cure of patients is the targeted elimination of the leukaemia’s starting cells, called leukaemia stem cells. “For therapy, we need to find the cause of the problem and tackle the leukaemia stem cells,” says Dr. med. Simon Raffel, project partner from the Department of Haematology, Oncology and Rheumatology (Medical Director: Prof. Dr. Carsten Müller-Tidow) at UKHD. Like healthy stem cells, leukaemia stem cells are located in the stem cell niche in the bone marrow and are able to constantly produce new leukaemia cells (blasts). The interaction of leukaemia stem cells with other factors and cells of the stem cell niche is not yet fully understood. This is where the currently approved junior research alliance comes in, which comprises three sub-projects: the analysis of single leukaemia stem cells, an investigation of the stem cell niche in the bone marrow, and a systems medical, comprehensive evaluation of the collected data.
In the stem cell niche, healthy and non-functional blood cells thrive equally
Dr. Simon Raffel from UKHD, in cooperation with Dr. Lars Velten of the Centre for Genomic Regulation (CRG), in Barcelona, Spain, will investigate the characteristics of leukaemia stem cells of AML patients in comparison with healthy blood cells. For this purpose, patient cells are isolated and surface markers, specific mutations, cell functions, and special metabolic properties of diseased cells are compared to healthy cells.
The leukaemia stem cells are located in the patient’s bone marrow – in the stem cell niche – which contains a diverse range of cells, such as immune, blood vessel, and connective tissue cells. To investigate their contribution to the development of leukaemia and resistance to therapy, the project coordinator and project leader Dr. Simon Haas (HI-STEM/DKFZ) will develop novel single-cell and spatially resolved analysis methods and use them to systematically investigate the AML microenvironment. “With our work, we hope to gain a better understanding of the pathogenesis and therapy resistance mechanisms of AML as a whole, which in the medium term will lead to new diagnostic and therapeutic options,” says Simon Haas.
In the third sub-project, the data collected using different methods will be evaluated by physicist and mathematician Dr. Laleh Haghverdi from EMBL. She will develop new bioinformatics methods and algorithms for integration and analysis in a systems biology approach. “Previous studies have looked at individual aspects of leukaemia cells, be they DNA mutations, RNA, or metabolic factors. We are now specifically aiming to use a comprehensive approach to investigate the interaction of multiple aspects of AML,” she explains.
Fighting leukemia cells, sparing healthy cells
The researchers are particularly interested in being able to better distinguish between healthy and leukaemia stem cells, as this is only possible to a limited extent using existing markers. Only when this can be done more precisely can new biomarkers for the discovery of the mutated cells be identified, opening up possible new points of attack for targeted therapies. “The treatment of AML will be all the more successful the more precisely we can specifically eliminate the leukaemia’s starting cells and spare the healthy blood cells in the future,” says Simon Raffel.
The funding of the junior research alliance LeukoSyStem by the German Federal Ministry of Education and Research (BMBF) enables the young scientists from Heidelberg to carry out interdisciplinary research in systems medicine. The project started at the beginning of 2020. The total funding amounts to approximately €2.45 million over five years, with a share of approximately €1.3 million for the Department of Haematology, Oncology and Rheumatology at UKHD.
The development of normal, healthy blood cells starts from haematopoietic stem cells in the bone marrow and proceeds through various stages of so-called precursor cells. In each of these stages, the accumulation of mutations can lead to cell degeneration and the development of blood cancer (leukaemia).
Related links
Department of Haematology, Oncology and Rheumatology at Heidelberg University Hospital
HI-STEM: The Heidelberg Institute for Stem Cell Technology and Experimental Medicine
LeukoSyStem
2,45 Millionen Euro zur Erforschung von Ursachen und Therapie bei Leukämie
Der Heidelberger LeukoSyStem-Verbund erforscht Leukämiestammzellen bei akuter myeloischer Leukämie (AML). Das Bundesministeriums für Bildung und Forschung unterstützt diese Kooperation desUniversitätsklinikums Heidelberg, HI-STEM (Deutsches Krebsforschungszentrum) und des Europäischen Laboratoriums für Molekularbiologie. Dies ist eine gemeinsame Pressemitteilung des Universitätsklinikums Heidelberg, des Deutschen Krebsforschungszentrums und des Europäischen Laboratoriums für Molekularbiologie.
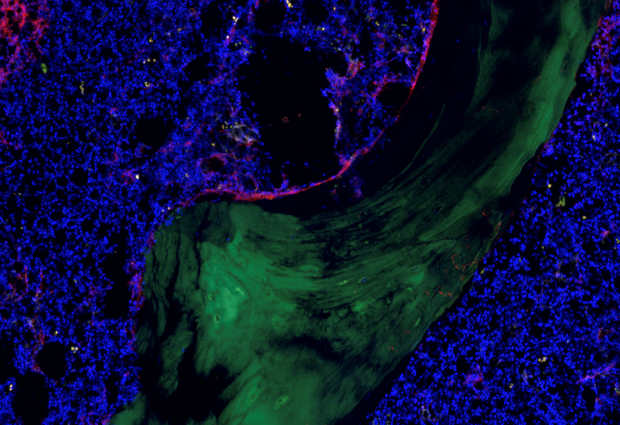
Leukämiestammzellen gelten als Ausgangspunkt einer Leukämie; ihre Eliminierung ist Grundvoraussetzung für eine langfristig erfolgreiche Therapie. Wissenschaftlerinnen und Wissenschaftler des Universitätsklinikums Heidelberg (UKHD), des Heidelberger Instituts für Stammzelltechnologie und Experimentelle Medizin im Deutschen Krebsforschungszentrum (HI-STEM/DKFZ) und des Europäischen Laboratoriums für Molekularbiologie (EMBL) konnten nun im Rahmen des Junior-Verbundes LeukoSyStem eine Forschungsförderung des Bundesministeriums für Bildung und Forschung (BMBF) in Höhe von 2,45 Millionen Euro einwerben. Ziel ihres Projektes ist es, die Ursprungszellen der akuten myeloischen Leukämie (AML) zu erforschen und auf diese Weise das Übel sozusagen „bei der Wurzel“ zu packen. Die Wissenschaftler wollen anhand von isolierten Einzelzellen aus Patientenproben charakteristische Marker, Mutationen, Funktionsdaten und Stoffwechselwege untersuchen, um Leukämiestammzellen und ihre Umgebung im Knochenmark besser verstehen zu können. Die gesammelten Daten sollen mithilfe neu zu entwickelnder Computer-Algorithmen übergreifend ausgewertet werden.
Leukämische Stammzellen als Ursache einer häufig tödlich verlaufenden Krankheit
Die Entwicklung normaler, gesunder Blutzellen geht von hämatopoetischen Stammzellen im Knochenmark aus und verläuft über verschiedene Stadien sogenannter Vorläuferzellen. Dabei kann es in jedem dieser Stadien durch Anhäufung von Mutationen zur Entartung von Zellen und der Entwicklung von Blutkrebs (Leukämie) kommen.
Die akute myeloische Leukämie (AML) ist die häufigste Form der Leukämie im Erwachsenenalter, bei der mutierte, funktionslose Blutzellen, sogenannte Blasten, die anderen Knochenmarkszellen überwuchern. In Europa erkranken jährlich drei bis fünf Patienten je 100.000 Einwohner an AML. Trotz Therapiemöglichkeiten wie Chemotherapie und Stammzelltransplantation kommt es häufig zu Rückfällen und die Fünf-Jahres-Überlebenswahrscheinlichkeit für Patienten unter 60 Jahren liegt bei 35 bis 40 Prozent und für Patienten über 60 Jahren bei nur fünf bis zehn Prozent.
Als Grundvoraussetzung für eine effektive Heilung der Patienten gilt die gezielte Eliminierung der Ausgangszellen der Leukämie, den sogenannten Leukämiestammzellen. „Zur Therapie müssen wir die Ursache des Problems finden und die leukämischen Stammzellen angehen“, sagt Dr. med. Simon Raffel, Projektpartner von der Medizinischen Klinik für Hämatologie, Onkologie, Rheumatologie (Ärztlicher Direktor: Prof. Dr. Carsten Müller-Tidow) des Universitätsklinikums Heidelberg. Die Leukämiestammzellen befinden sich wie die gesunden Stammzellen auch in der Stammzellnische im Knochenmark und sind in der Lage, ständig neue Leukämiezellen (Blasten) zu bilden. Das Zusammenspiel von Leukämiestammzellen mit anderen Faktoren und Zellen der Stammzellnische ist noch nicht ausreichend geklärt. Hier setzt das aktuell bewilligte Juniorverbund-Projekt an, das drei Teilprojekte umfasst: die Einzelzellanalyse leukämischer Stammzellen, eine Untersuchung der Stammzellnische im Knochenmark und eine systemmedizinische, übergreifende Auswertung der gesammelten Daten.
In der Stammzellnische gedeihen gesunde und funktionslose Blutzellen gleichermaßen
Dr. Simon Raffel vom Universitätsklinikum Heidelberg wird in Kooperation mit Dr. Lars Velten (Centre for Genomic Regulation, Barcelona, Spanien) Charakteristika von Leukämiestammzellen von AML-Patienten im Vergleich zu gesunden Blutzellen untersuchen. Hierzu werden Patientenzellen isoliert, vereinzelt und Oberflächenmarker, spezifische Mutationen, Zellfunktionen sowie spezielle Stoffwechseleigenschaften der kranken im Vergleich zu den gesunden Zellen betrachtet.
Die Leukämiestammzellen befinden sich im Knochenmark des Patienten in der so genannten Stammzellnische, deren Milieu durch weitere Zellen wie Immun-, Blutgefäß- und Bindegewebszellen geprägt ist. Um deren Beitrag an der Entstehung und Therapieresistenz von Leukämien genauer zu erforschen, wird der Projektkoordinator und Teilprojektleiter Dr. Simon Haas (HI-STEM/DKFZ) neuartige Einzelzell- und räumlich-aufgelöste Analysemethoden entwickeln und mit Hilfe dieser das AML Mikromilieu systemisch untersuchen. „Mit unseren Arbeiten möchten wir die Pathogenese und Therapieresistenzmechanismen der AML in ihrer Gesamtheit besser verstehen lernen, was mittelfristig zu neuartigen Diagnose- und Therapieoptionen führen soll“, fasst Simon Haas zusammen.
Die mit verschiedenen Methoden gesammelten Daten werden im dritten Teilprojekt von der Physikerin und Mathematikerin Dr. Laleh Haghverdi vom EMBL ausgewertet. Hierfür wird sie neue bioinformatische Methoden und Algorithmen zur Integration und Analyse im Sinne eines systembiologischen Ansatzes entwickeln. „In bisherigen Untersuchungen wurden einzelne Aspekte der Leukämiezellen betrachtet, seien es DNA-Mutationen, RNA oder metabolische Faktoren. Wir zielen nun speziell darauf ab, mit einem übergreifenden Ansatz das Zusammenwirken multipler Aspekte der AML zu untersuchen“, erklärt Laleh Haghverdi.
Ausgangszellen der Leukämie bekämpfen, gesunde Zellen schonen
Besonders eine bessere Unterscheidung von gesunden und leukämischen Stammzellen ist den Forschern wichtig, da diese anhand bisheriger Marker nur begrenzt möglich ist. Nur mit einer genaueren Differenzierung lassen sich neue Biomarker zur Entdeckung der mutierten Zellen und damit Angriffspunkte für eine gezielte Therapie herausfinden. „Die Behandlung der AML wird umso erfolgreicher, je genauer wir in Zukunft spezifisch die Ausgangszellen der Leukämie eliminieren und die gesunden Blutzellen verschonen können“, so Simon Raffel.
Mit der Förderung des Juniorverbunds LeukoSyStem durch das Bundesministerium für Bildung und Forschung (BMBF) erhalten die Heidelberger Nachwuchswissenschaftler die Möglichkeit, Forschungsarbeiten zur Systemmedizin interdisziplinär zu realisieren. Das Projekt startet Anfang 2020, die Gesamtfördersumme beträgt ca. 2,45 Mio. Euro für fünf Jahre, mit einem Anteil von rund. 1,3 Mio. für die Medizinische Klinik für Hämatologie, Onkologie, Rheumatologie des UKHD.
Weiterführende Links
Abteilung für Hämatologie, Onkologie und Rheumatologie der Universitätsklinik Heidelberg
HI-STEM: Heidelberger Institut für Stammzelltechnologie und Experimentelle Medizin
LeukoSyStem



